Leadership
- Associate Professor Jonathan Barrett
- Dr Con Giannellis
- Associate Professor Nerina Harley
- Dr Bryan Lashansky
- Dr Laven Padayachee
- Dr Simon Reilly
- Dr Zia Ansari
- Dr Matt Ryan
- Dr Iain Duncan
- Dr Nicole Tan
- Dr Jennifer Mines
Highlights
Emergency Department
- Accredited for advanced trainees in emergency medicine for a 12-month period
- Actively involved in research
- Extremely low bypass rate
- Features a purpose-designed clinical space with the best of medical technology to treat patients with serious conditions and an experienced team of emergency medicine professionals.
- Higher rate of emergency physician specialists working in Epworth Emergency Department compared to other hospitals’ emergency departments.
- Most specialties covered with a comprehensive on-call roster
- Teaching Hospital: Medical students on rotation from Monash and Melbourne Universities
Intensive Care
- Epworth admits approximately 3,000 patients to our four state-of-the-art intensive care units each year at Epworth Eastern, Epworth Freemasons, Epworth Richmond and Epworth Geelong.
- Epworth Richmond ICU consists of 26 private rooms, providing patients with privacy and a quiet recovery environment. Each room features the latest medical equipment for monitoring patient conditions, as well as switchable glass that is transparent to enable monitoring but can be switched to opaque when privacy is required
- Epworth Geelong ICU also has a state-of-the-art facility supporting the activities of our newest major hospital.
Anaesthetics
Anaesthesia
- Epworth delivers anaesthesia and sedation for over 80,000 patients per year in 54 operating theatres over 5 campuses.
- Anaesthesia is delivered for a huge range of procedures from small excisions under local anaesthesia and sedation to complex Open Heart, Neurosurgical and Orthopaedic procedures.
- We are involved in anaesthesia for Robotic Surgery, Cancer Surgery, Obstetric procedures, IVF and many other types of procedures across our campuses.
Our performance
Emergency Department
|
Average waiting time to see a doctor* |
37 minutes |
* In private hospitals this includes triage and provision of financial information.
Comment: We see 100% of critically unwell patients immediately and meet time targets for other categories of urgency
Intensive Care
To measure our performance, our intensive care results are compared with other hospitals participating in the Centre for Outcome and Resource Evaluation (CORE) hosted at the Australian and New Zealand Intensive Care Society.
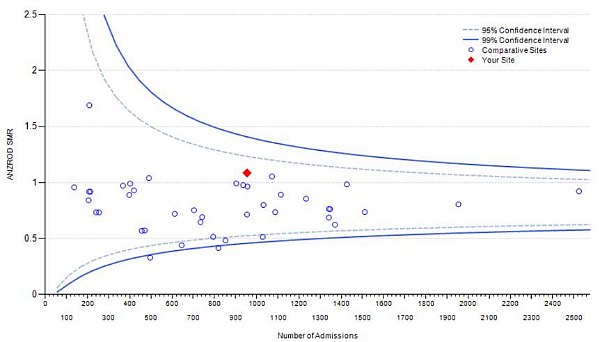
A key measure of success in intensive care is the proportion of patients who survive. There are a significant amount of factors affecting an individual’s risk of a poor outcome. As a result, risk adjustment is used to take into account factors affecting potential patient outcome so that a fair comparison between hospitals can be made.
Benchmarking can then be undertaken using a standardised mortality rate (SMR), where an SMR of 1 is the expected outcome for a patient of a particular condition and clinical risk; and less than 1 a better than expected outcome.
Activity
Services
-
a
-
b
-
c
-
d
-
e
-
f
-
g
-
h
- i
-
j
-
k
-
l
-
m
-
n
-
o
-
p
-
q
-
r
-
s
-
t
-
u
-
v
-
w
-
x
-
y
-
z
