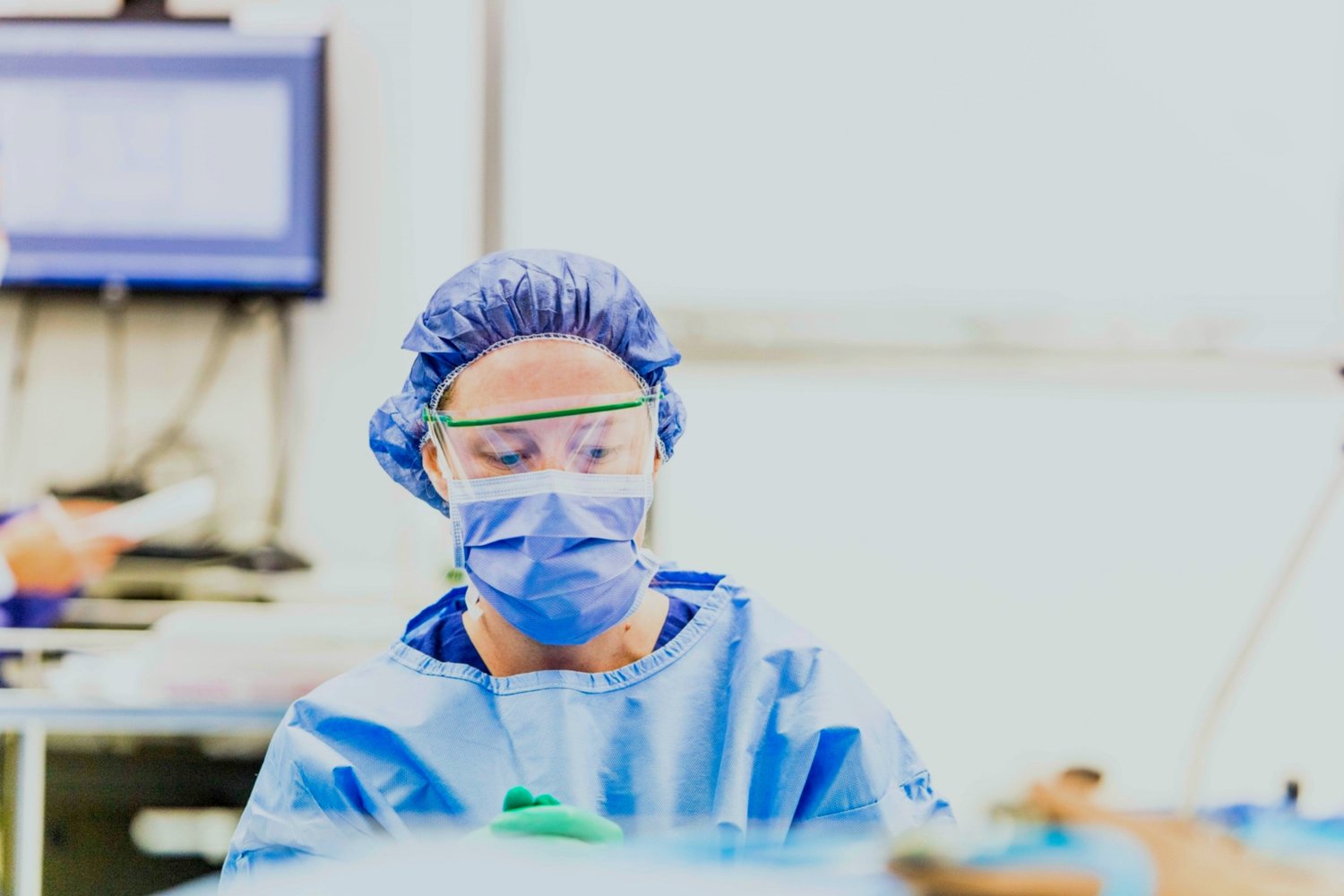
Molecular pathology techniques are used to diagnose all blood cancers including myeloma, leukaemia and lymphoma.
Pathology testing also shows how a person is responding to a novel treatment during clinical trials, and for patients who may have exhausted other options, access to these treatments can be lifesaving.
Snowdome funds projects based at several different institutions including the Peter MacCallum Cancer Centre and Epworth HealthCare.
Nicole Brooks, Research Program Manager, Molecular Oncology and Cancer Immunology Department (MOCI) Epworth HealthCare said;
“As researchers, we want to ask more questions and as a result of the efforts of the Snowdome Foundation, Epworth Medical Foundation and other philanthropic organisations we are in a fortunate position to continue our research efforts.
“Our research is not just tinkering in the lab in the way many people might think. Rather, a group effort to provide desperate patients an alternative option and when we can prove that something is actually working, we can then make a case to get access to new drugs for more patients.”
As cancer therapy is increasingly delivered as precision treatment, this requires precision diagnostics.
Dr Piers Blombery is a Consultant Haematologist and medical lead of Peter Mac’s Molecular Haematology Laboratory. This lab runs an Australia-wide genomic testing service which from a blood sample can identify genes or genetic irregularities known to drive cancer.
“For the patient it’s no more difficult than a standard blood test, and the information we get is very powerful in guiding and personalising their treatment.”
“It often means we can rule out approaches that won’t work, or will have a very poor response, and instead go down treatment pathways that should get the best results.”
For example, every year about 1000 Australians are diagnosed with chronic lymphocytic leukaemia (CLL). Genomic testing can reveal whether these patients have either an IGHV or TP53 gene irregularity.
Both are clinically important. CLL patients with an IGHV irregularity respond well to standard chemo-immunotherapy, and this treatment can give them long-term remissions.
“Alternatively, we also know CLL patients with a TP53 irregularity will likely have a very poor response to standard chemo-immunotherapy,” Dr Blombery says.
“These patients do better on novel agents such as BTK inhibitors or BH3-mimetic agents which are currently accessible through clinical trials or compassionate access programs.”
“It is genomic testing that allows us to find these irregularities and ensure patients get the treatments most likely to work for them.”
Dr Blombery also said when performing genomic testing, new clinically important gene irregularities can be discovered. These are passed to researchers who are looking to better understand the fundamental drivers of cancer.
“The more of these gene irregularities we know of, the more we can develop potential new anti-cancer drugs and also personalise treatments so patients have better outcomes.”
“Based on international evidence, we know that patients have better outcomes on clinical trials, but many people will be unaware that due to our small population, Australian patients are rarely included in blood cancer trials.”
“That is the mission of Snowdome, to ensure more early phase clinical trials are initiated here in Australia.”
“The type of research we fund is not confined to the laboratory, but relies on pathology testing to monitor success and manage patient welfare, as well as the development of companion diagnostic tests that are the gateway to novel therapies.”
29 July 2019