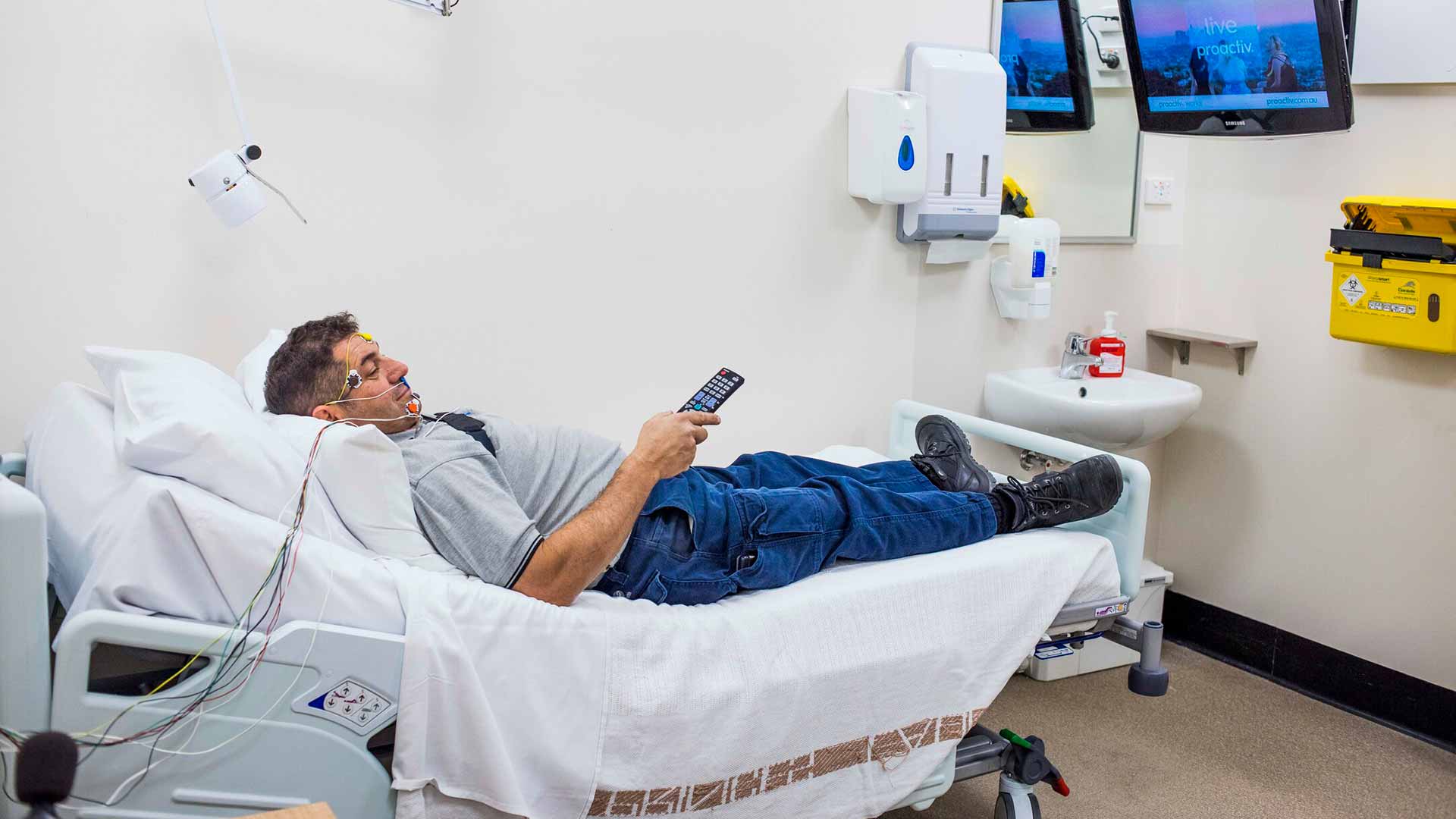
A deep, uninterrupted and refreshing sleep is essential for optimal everyday functioning. But for those with sleep apnoea, maintaining a solid sleep state is impossible and the effects can be frustrating.
Sleep apnoea is broadly defined as a condition where the cessation of breathing occurs during sleep and it can be categorised into either obstructive or central. Whilst it’s important to be aware that there are different kinds of apnoea, obstructive sleep apnoea (OSA) is the most common type and is the focus of this blog post. Notably, research reveals one in ten Australians suffer from undiagnosed OSA!
OSA occurs when the throat walls partially or completely come together during sleep, blocking the pathway of air. When this occurs, those with sleep apnoea will stop breathing. The brain will sense an absence of breathing or a decreased oxygen level, triggering a brief period of wakefulness. Sufferers will immediately fall back asleep and are often unaware about these episodes, or apnoeas, which they experience nightly.
Group sleep services manager at Epworth, Darrel Wicks uses a thick shake and straw analogy to explain what happens in OSA patients.
“If you’ve got a thick shake and you’re sucking that thick shake through a straw – if you suck too hard, the straw will collapse. That’s exactly what happens in your upper airway with obstructive sleep apnoea. It’s pressure differentials causing the upper airway to collapse which is the same dynamics of sucking on a straw too hard.”
Anatomic abnormalities are a major cause of OSA – this includes large tonsils, a large uvula, narrowed windpipes, a goitre or a recessed jaw. According to Mr Wicks, obesity should be viewed as more of an “exacerbating factor”, rather than a cause.
Mr Wicks also says the two major symptoms associated with OSA are snoring and excessive daytime sleepiness. Other symptoms may include mood changes, poor concentration and the need for frequent urination during the night. Alarmingly, untreated sleep apnoea increases the risk of hypertension, stroke, diabetes, depression and accidents.
In terms of the severity, individuals can experience varying levels of OSA which is classified according to the number of interruptions during the night. Mild OSA is where five to 15 interruptions occur per hour, moderate is 15 to 30 and severe is more than 30.
For a diagnosis of OSA, polysomnography is needed. The severity will then inform which treatment is required. For mild cases – sleep apnoea pillows, weight loss, reducing alcohol and quitting smoking may improve symptoms. For moderate to severe OSA, the gold-standard of treatment is continuous positive airway pressure therapy (CPAP).
“CPAP is non-invasive, and it is extremely effective across all of the ranges. The only downside it has is tolerance and compliance.”
For cases where conservative treatments are unsuccessful, and patients struggle to adhere to CPAP – mandibular advancement splinting, and surgery are also available. There are various surgical procedures available, and the best option is explored with an otolaryngologist as a final treatment option.
If you are concerned that you may have OSA or another sleep disorder, please visit the following link regarding Sleep Services at Epworth.
21 March 2021